Volume 14, 2008
A Community Development Approach to Rural Recruitment
C. Ken Shannon
Contents
Abstract
Introduction
Development of the RCP
Structure and Operation of the RCP
RCP Implementation and Experience
Discussion
Conclusions
References
Acknowledgments
About the Author
Abstract
Programs designed to empower rural communities for health care provider recruitment have usually focused on the health care sector without aggressively addressing broader community development issues. The Recruitable Community Project (RCP) in West Virginia includes community education on recruiting and also assessments of and recommendations to rural communities on broad-based community development, aiming to enhance communities' recruiting potential. The project provides multidisciplinary university-based planning assistance programs for small communities, involving collaborative community visits. The project also uses a project manager as a "community encourager" who participates in community education and in the formulation of sustained community recruiting efforts. From August 1999 through August 2001, 7 underserved rural communities completed the RCP organizational processes and hosted planning assistance teams. Members of community recruitment boards gave high marks to the RCP process, its planning assistance teams, and its usefulness in establishing community ties to state and academic agencies. Since working with the RCP, the 7 communities have recruited 27 providers, success possibly stimulated by their RCP involvement (data current as of September 2002). This model of community training and development to empower rural communities to better recruit health professionals shows early promise. This model could be broadened to include more collaboration of community development and health science disciplines programs for recruitment and retention efforts.
Introduction
Small rural communities have long had difficulties recruiting health care providers. The role of rural communities in the recruiting process has been uncertain, and rural community members have traditionally lacked experience in recruiting, often not addressing links between community development and recruiting potential. Programs designed to enhance community decision-making in health care [1-9] have involved sectors other than health care to a varying degree, although the interrelationships of health care services and the local economy have been acknowledged [10-12]. Several programs, including those of national organizations such as the Cooperative Extension Service and the National Rural Development Partnership, have included health care system topics in community development initiatives, although not specifically for enhancement of recruitment. There have been calls for and examples of academic outreach programs that benefit community health status and include elements of community development [13,14], but these have not included a deliberate community development effort focused on enhancement of the community's recruiting potential.
Links between prospective providers and rural communities in need of health care providers have not traditionally been strong. Residency training programs in this country have not always addressed the problems that the recently graduated prospective provider may face in a rural location nor have they uniformly assisted the provider in the transition from an academic to a rural setting [15-17]. Lifestyle and cultural issues have been important in rural recruitment [18-21], but there is no consensus on how these issues should be addressed or whether a combined community development and education effort may have utility in making underserved rural communities more attractive to health care providers or in promoting community recruiting readiness.
West Virginia is a poor rural state with many unmet health care needs. Fifty of 55 counties have medically underserved areas (MUAs) or health professional shortage areas [22] despite the presence of 3 medical schools and multiple rural training sites for health professions students. As in other states, these MUAs are generally economically disadvantaged areas. The economic picture is not likely to change substantially in the near future. Furthermore, there have been reports of a decrease in the number of physicians in the state due to a variety of factors. It is, therefore, essential that West Virginia develop new approaches to enhance rural recruitment to help avoid a worsening shortage of providers.
The purpose of this article is to describe an innovative approach developed in response to West Virginia's rural health care provider recruitment needs. The Recruitable Community Project (RCP) is centered on an effort to promote general community development, leadership, and education. Based on the premise that rural community recruitment potential is correlated with general community development and a proactive community effort, the RCP combines the efforts of a project-sponsored "community encourager" [1,6], university-based community planning assistance programs [23-26], and health care provider recruitment initiatives.
Development of the RCP
The RCP was implemented in late 1998 by faculty of the Department of Family Medicine at West Virginia University (WVU). Faculty collaborated with state agencies, university departments, and community assistance teams before funding application and during implementation of the project. Two of these university-based assistance teams (the First Impressions Program (FIP) and the Community Design Team (CDT)), which already had been addressing various issues of community development in the state, were integrated into the RCP. With this, suggestions regarding general community development outside traditional health care topics were available to RCP communities. Thus, the RCP design represented a new model to help train community members on barriers to successful provider recruitment, broad-based community development, and sponsoring elective rural clinical rotations for primary care trainees. The community assistance teams function through the efforts of volunteers from various institutions, agencies, and communities and are founded on the strong service commitment of West Virginia's academic departments and agencies. The use of these community assistance teams allowed investigation of the basic RCP premise that health care provider recruitment to rural communities can be enhanced through general community development.
The RCP design is based on the assumptions that (1) health care personnel are attracted by a community's physical attractiveness, local supports for the practice and family, and the welcome they feel; (2) communities do not understand what health care personnel are looking for or how their community is perceived by potential recruits; (3) communities can learn and can effect positive changes; (4) outside assistance from trusted in-state resources can provide this needed assistance; (5) assistance is best delivered in a supportive and collaborative fashion; and (6) an explicit recruitment plan serves as a good vehicle through which to focus the community's efforts.
Funding for the RCP, as a demonstration project, was initially secured from the Claude Worthington Benedum Foundation in 1998. With the advent of the West Virginia Rural Health Access Program (WVRHAP) in 1999, a component of the Robert Wood Johnson Foundation's Southern Rural Access Program that operates in 8 southern states, RCP funding was supplied entirely by the WVRHAP. The WVRHAP derives its funding from both the Robert Wood Johnson Foundation and Claude Worthington Benedum Foundation. Funding covers costs of project personnel and travel, administrative costs of the community assistance teams (total of $3500 for each RCP community), and a stipend for primary care trainees who elect 1-month rural rotations to sites approved by project personnel.
Structure and Operation of the RCP
The project is directed by a multidisciplinary project oversight committee, which is composed of personnel from West Virginia agencies involved in recruitment and retention, private and community organizations, and various academic departments. Project personnel include a physician with rural West Virginia practice experience, a project manager with community programs experience, and a part-time secretary.
The RCP functions in a sequential fashion. Initially, information regarding the RCP was distributed throughout West Virginia through a statewide rural training network, the Cooperative Extension Service, and mailings to chambers of commerce and health care facilities. Ongoing efforts include an informational brochure and Web site that outline the program and the application process. The RCP program manager then visits interested communities and assists community members in supplying the required information regarding community eligibility for project entry.
Eligibility criteria include the following: (1) location in an underserved rural area; (2) demonstrated ability to organize for a recruitment effort (formation of a recruitment board composed of key community members); (3) willingness to prepare for and host the community assistance teams; (4) perceived ability by community and project personnel of community ability to support a viable practice; and (5) identification of a sponsor, such as a hospital or clinic, that would offer a contract to a prospective recruit. On the basis of available information, the project oversight committee then annually selects 2 or 3 RCP communities.
After project entry, RCP communities then perform further self-assessment and the recruitment board works with project personnel, learning of barriers to recruitment and positive initiatives that communities may use to help overcome barriers and to build community capacity. The RCP project manager serves as an encourager to several communities, traveling frequently to the RCP communities, providing one-on-one consultation and assistance, conducting community workshops, and helping communities to plan their recruitment effort and to prepare for visits from community assistance teams. The latter requires extensive community assessment and information collection.
The RCP includes an early educational initiative that focuses on enhancement of recruiting knowledge and abilities of rural community leaders. Many community recruitment board members experienced their first opportunity to learn of important recruitment issues, such as practice viability, practitioner debt, and lifestyle issues, through their involvement with the RCP. Educational tools for communities have been developed, including a short recruitment manual, a video on recruitment and retention, and a board game that introduces community members to the hurdles and pitfalls associated with rural medical practice and the important contributions communities can make to the success of a practice and to the retention of practitioners [27].
In addition to building the capacity of participating communities to recruit interested practitioners, the RCP also works to link practitioners and communities through other efforts. The RCP linkage efforts include sponsoring funded trainee rotations in any underserved rural West Virginia community that is recruiting, presenting information at primary care training sites, and sponsoring opportunity fairs where prospective recruits can interface with community members.
One of the essential components of the RCP is the community assistance offered by multidisciplinary community assistance teams that are administered from academic departments at WVU. These teams incorporate expertise from various agencies, institutions, and communities and are valuable as outside resources that can assist a community in self-assessment and in suggesting initiatives for community development. These teams have historically had a role in various community assessment and development activities and their continuation is based on the strong service commitment of academic departments and state agencies in West Virginia. When incorporated into the RCP process, these teams also assume additional functions by assessing the local health care system and making recommendations for improvements, particularly those involving recruitment of primary health care providers.
One such community assistance program is the WVU FIP [23,24]. The FIP has supported community assessment at WVU since 1997 and has visited approximately 20 West Virginia communities. The FIP team is composed of approximately 5 volunteers who independently visit the community as anonymous first-time visitors and later present to the community their impressions of the town and their recommendations about ways to improve appearances and avoid negative first impressions. The FIP team members gain their impressions by driving around the community and talking to community members. The team formulates this information into a written report that is made available to the community and to a subsequent planning team, the CDT.
The WVU CDT [25,26] visits the community for a more comprehensive effort, resulting in recommendations in various areas of community development. The CDT has been functional since 1997 and has visited approximately 20 communities throughout the state. It has addressed a variety of individual community development issues that have been identified by the community, by the FIP, or through the required application process. The CDT is typically composed of 12 to 20 volunteers from West Virginia agencies, communities, and academic departments, representing a variety of disciplines, such as engineering, public administration, landscape architecture, historical preservation, extension services, community economic development, and recreation.
When functioning as a component of the RCP effort, the CDT also addresses issues of health care access, particularly recruitment of health care providers, previously detailed through the RCP process of community interaction. In RCP communities, the CDT also includes the RCP physician project director, project manager, and personnel from health care disciplines such as family medicine and community medicine. Community members host these CDT members during a 3-day community visit when community input is sought, collaborative assessment and planning are performed, and general recommendations are made for community development and recruitment.
The community provides input through the host families, presentations by community members to the CDT, and a community forum typically held in the evening at a local facility. The most pressing issues challenging the community are identified. The CDT members are assigned to various groups to suggest possible solutions and collaboratively develop recommendations on each topic. The CDT groups present their findings and recommendations to the community at the end of the visit and subsequently submit a written report to the community and county leaders. The topics most often addressed have involved health care and economic development, including community-specific topics such as community revitalization and leadership, transportation, recreation, tourism, and historical preservation. Follow-up consultations and site visits by CDT members are provided as needed. (Figure 1 provides an outline of the RCP community process.)
Figure 1:
Recruitable Community Project (RCP) Community Process
| Community Education, Recruitment Board Formation | Community FIP Visit | |
 |
 |
|
 |
||
| Community FIP Report, Preparation for CDT Visit | ||
 |
||
| Community CDT visit, Recommendations | ||
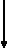 |
||
| Follow-up by RCP, CDT personnel | ||
RCP Implementation and Experience
As of September 2002, 12 communities had submitted applications and 7 were selected to participate in the RCP. All 7 RCP communities are rural, with populations ranging from 400 or more to nearly 4500, and are located in MUAs. As of August 2001, all 7 had completed the self-assessment, convened a recruitment board, and hosted the 2 planning assistance teams. Since the RCP is too new to assess its long-term successes, only early experiences and outcomes are described.
As of September 2002, these 7 communities had recruited a total of 27 health care providers, including 14 physicians, 6 nurse practitioners, and 7 physician assistants since their entry into the RCP. Given that rural rotations have traditionally been a major effort to improve rural recruitment, it is noteworthy that only 2 of these recruits had participated in an RCP-sponsored rural rotation, thus highlighting the role of these communities in proactive recruitment of providers who had not performed a local RCP clinical rotation.
An anonymous survey of community recruitment board members has provided early evidence of program success from the perspective of those respondents. Of 25 board members surveyed, the 17 respondents rated the value of the FIP, CDT, and overall RCP process to community development, attitudes, knowledge, and recruiting potential. High numerical ratings and positive comments were given to each program. High value was placed on the FIP in promoting awareness of community appearance, development, and leadership issues. The CDT was valued for increasing the level of community interest in development, leadership, and recruitment issues; increasing the level of interest of county leadership in development issues; and promoting a positive community attitude toward the academic institution (WVU) as a partner in development issues. The overall RCP process was given high marks for promotion of community knowledge of and readiness for recruitment, personal leadership and cooperative skills, and a positive community attitude toward the academic institution.
Discussion
This report describes the RCP, a unique approach to enhance the recruiting potential of rural Appalachian communities through general community development, including enhancement of community knowledge on health care and recruiting issues. The use of community assistance teams for the purpose of enhancing recruiting ability through broad-based community development initiatives is the most unique aspect of this program. General community development is closely related to economic issues and seems to be an important issue for maintenance of health care services. A common problem cited by RCP communities was the exodus of potential patients to more "developed" communities.
Intuitively, it would seem that a rural community that proactively prepares for recruitment by actively engaging in community development activities intended to improve the health of its community is more likely to be successful in its recruitment efforts. The RCP attempts to assist communities in making a positive impression on prospective recruits and in addressing barriers to rural recruitment by promoting community readiness for recruitment through educational processes and general community development. These barriers are addressed through a sequential process of proactive community training and development. The RCP communities had some successes in recruiting providers after completing the processes of organization for recruitment and the hosting of the community planning assistance programs. Aside from any recruitment issues, the community perception of strengthened readiness for development has been an evident outcome. The program has also strengthened links between communities and academic and state agencies.
The success of programs such as the RCP depends on a number of factors: (1) community interest in proactive efforts in recruiting (interest was ascertained in this project by evidence of completion of application materials and through meetings involving community and project personnel); (2) the role of the project manager as an encourager and resource for sustained community efforts (the importance of this has been evident); and (3) the collaborative efforts involving community, state, and academic partners. With an atmosphere of cooperation initially established by interaction of community and project personnel, the small Appalachian communities have been receptive to recommendations from outside personnel and agencies, and the communities have often acted on these recommendations.
Preliminary evidence suggests that community efforts in adopting a proactive stance in community development and recruiting can attract health care providers. Although more complex and labor intensive, these efforts may be more effective in rural recruiting than are the efforts in supporting rural RCP rotations for trainees.
This model for enhancing rural community recruiting potential could be used on a wider scale in other states and regions of the country where commitments for funding and multidisciplinary collaboration can be secured. State agencies and large academic institutions commonly have existing community development programs; promotion of multidisciplinary input into such programs, including that of experienced rural practitioners, could allow recruitment initiatives similar to those of the RCP. Project initiatives could be expanded to involve a more developed collaborative program that integrates traditional community planning and development programs with input from rural health care providers, training programs, health care workforce planners, and consultants, so that stronger initiatives could be more tailored to the requirements of the recruiting site.
There are limitations to evaluation of this model at this preliminary stage. The effect of community development initiatives in stimulating recruitment successes is unknown and needs more study. More experience with a larger number of communities and more information on recruits are needed for a more complete evaluation. No assessments of practice obligations or of retention of recruits has yet been completed. There has not been enough experience with the model to allow a comparison with a control group of communities, although it is known that past recruitment into rural West Virginia has traditionally been difficult.
Conclusions
As a program to stimulate recruitment of health care providers by rural communities in West Virginia, the RCP has shown some preliminary successes. The attempted enhancement of rural community recruiting potential through processes of community education and general community development may have utility in promoting rural health care provider recruitment, but more study is needed. The use of university-based planning assistance programs in community development for enhancement of rural recruitment is the most unique aspect of the RCP program. These community efforts may be more effective in promoting rural recruiting than are RCP efforts in supporting rural rotations for trainees. This approach to rural recruitment may be enhanced through further collaboration of traditional community planning and development programs with health care workforce initiatives. This approach may be tested through further evaluation of the RCP and through its implementation in other rural areas.
References
1. Amundson BA, Hagopian A, Robertson DG. Implementing a Community-Based Approach to Strengthening Rural Health Services: The Community Health Services Development Model. Univ of Washington, Seattle, WA: Washington, Alaska, Montana, Idaho (WAMI) Rural Health Research Center; 1991.
2. Amundson BA, Rosenblatt RA. The WAMI Rural Hospital Project, part 6: overview and conclusion. J Rural Health. 1991;7:560-574.
3. Fricker S, Evans S, Main K, Kepferle L, Myers JA. Community Rx. Forum Appl Res Public Policy. Summer 1998:106-109.
4. Iowa Department of Public Health. Hometown Health: Community-Based Health Planning. 2nd ed. Des Moines, IA: Iowa Bureau of Rural Health and Primary Care; 1999.
5. National Rural Health Association. Community Development Applied to Rural Health Care. Kansas City, Mo: National Rural Health Association; 1995.
6. National Rural Health Association. Community Solutions for Rural Health: An Empowerment Initiative for Rural Communities. Kansas City, Mo: National Rural Health Association; 1997.
7. Straub L, Schraith K. Rural Communities Making a Health Care Difference: What Can Be Learned. Macomb, III: Illinois Institute for Rural Affairs, Western Illinois University; 1994.
8. Veitch C, Harte J, Hays R, Pashen D, Clark S. Community participation in the recruitment and retention of rural doctors: methodological and logistical considerations. Aust J Rural Health. 1999;7:206-211.
9. Ludtke R, Cochran C, Geller J, Fickenscher K, Hart P. The ARCH demonstration project: enhancing rural health care through community development. Small Town. Jan-Feb 1989:15-21.
10. Cordes S, Doeksen GA, Shaffer R. Rural economic development and health services. In: Beaulieu J, Berry D, eds. Rural Health Services: A Management Perspective. Ann Arbor, Mich: Aupha Press/Health Administration Press; 1994:27-56.
11. Doeksen GA, Johnson T, Willoughby C. Measuring the Economic Importance of the Health Sector on a Local Economy: A Brief Literature Review and Procedures to Measure Local Impacts. Mississippi State, Miss: Southern Rural Development Center; 1997.
12. Rural Policy Research Institute. Operation Rural Health Works Briefing Report. Vol 1, No. 1. Columbia, Mo: Dept of Agriculture, Office of Rural Health Policy; 1998.
13. Kaufman A. Fostering the health of communities: a unifying mission for the University of New Mexico Health Sciences Center. Acad Med. 1996;71:432-440.
14. Foreman S. Social responsibility and the academic medical center: building community-based systems for the nation's health. Acad Med. 1994;69:97-102.
15. Borus JF. The transition to practice. J Med Educ. 1982;57:593-601.
16. Merkel WT, Walbroehl GS, Dimlich HS. The third-year resident rampage: a separation crisis of manageable proportions. J Med Educ. 1980;55:366-367.
17. Reuben DB, McCue, JD, Gerbert B. The residency-practice training mismatch: a primary care education dilemma. Arch Intern Med. 1988;148:914-919.
18. Costa AJ, Schrop SL, McCord G, Gillanders WR. To stay or not to stay: factors influencing family practice residents' choice of initial practice location. Fam Med. 1998;8:214-219.
19. Holmes JE, Miller DA. Factors affecting decisions on practice locations. J Med Educ. 1986;61:721-726.
20. Leonardson G, Lapierre R, Hollingsworth D. Factors predictive of physician location. J Med Educ. 1985;60:37-43.
21. Schwartz RW, Jarecky RK, Strodel WE, Haley JV, Young B, Griffen WO. Controllable lifestyle: a new factor in career choice by medical students. Acad Med. 1989;64:606-609.
22. West Virginia Department of Health and Human Resources. West Virginia Medically Underserved Areas (MUAs). Charleston, WV: West Virginia Bureau for Public Health; 2001.
23. Lewis A, Schneider J. First Impressions: A Program for Community Assessment & Improvement. Madison, Wis: University of Wisconsin Extension Service; 1991.
24. West Virginia University Extension Service. First Impressions. 2001. Accessed Dec 2002. Available at: www.wvu.edu/%7Eagexten/crd/firstimp.htm.
25. Loveridge S. Keys to engaging faculty in service: Lessons from West Virginia's community design team. J Plann Educ Res. 2002,21:331-339.
26. Loveridge S, Plein C. Catalyzing local leadership and infrastructure development. In: Schaeffer P, Loveridge S, eds. Small Town and Rural Economic Development: A Case Studies Approach. Westport, Conn: Praeger; 2000:11-19.
27. West Virginia University. The Retention Game. 2002. Accessed Dec 2002. Available at www.hsc.wvu.edu/som/fammed/rcp_game/.
Acknowledgments
Thank you to the Journal of Rural Health for permission to reprint this paper (Vol. 19 # S: Supplemental 2003: Pages 347-352)
The Recruitable Community Project is funded by the Claude W. Benedum Foundation and the Robert Wood Johnson Foundation through the Southern Rural Access Program. The following individuals are acknowledged for their contributions in review and editing: Donald E. Pathman, MD, MPH, associate professor and research director of family medicine and co-director of the Program on Health Professions and Primary Care of the Cecil G. Sheps Center for Health Services Research, University of North Carolina at Chapel Hill; Elaine Mason, MEd, director of rural recruitment and retention at the West Virginia University School of Medicine; and James G. Arbogast, MD, professor and residency director, West Virginia University Department of Family Medicine. For further information, contact: C. Ken Shannon, WVU Department of Family Medicine, PO Box 9152, Health Sciences Center, Morgantown, WV 26506; e-mail shannonk@rcbhsc.wvu.edu
About the Author
Dr. Shannon has a background in rural WV primary care and is the Research Director in the WVU Department of Family Medicine. His research interests include the community role in recruitment of health care professionals, the rural training of health care discipline students and the role of practice-based research networking in rural areas.