COMM-ORG Papers
Volume 13, 2007
http://comm-org.wisc.edu/papers.htm
Participatory Research at Cooperative Care: Supporting Caregivers and Building a Unified Cooperative
Andrea
Robles and Julie Whitaker, with Louise (Mankowski) Randall, Donna Tompkins, Joan
Vroman, Vicki Walejko, and Margaret Bau
E-mail:
robles@ssc.wisc.edu
or whitaker.julie@gmail.com
Contents
Summary
Introduction
Homecare Workers and Cooperative Care
Worker Owned Cooperatives and Participatory Action
Research
Project Background
Organization of the Report
Caregiver Background
Cooperative Care Members
Working with Clients
Physical Equipment, Emergency Plans and Client Well-Being
Physical Equipment
Emergency Plans
Client Well-Being
Physical and Emotional Issues Faced by Caregivers
Physical Issues for Caregivers
Emotional Issues for Caregivers
Caregivers’ Suggestions for Building Communication and Cooperation among
Cooperative members
Gathering More Information About Clients
Establishing Communication Methods for Caregivers Who
Care for the Same Client
Creating More Opportunities for Cooperative Members to
Talk With One Another
Fostering an Environment Wherein Cooperative Members
Feel More Comfortable Communicating
With Cooperative Management and the Board Of
Directors
Actions
Cooperative Care Activities
Role of Participatory Research
Lessons Learned
Notes
List of Tables, Figures, and Boxes
About the Authors
Acknowledgements
This report is based on a participatory research project conducted between June 2003 and December 2004, and the subsequent actions inspired by it through June 2006. Members of Cooperative Care, a worker-owned home care agency, and two academic researchers conducted the research.
The research objectives were to learn: 1) how the cooperative could better support their members physically and emotionally; and 2) how to improve cooperation and communication among members. With the information obtained with this project, caregivers aimed to build a stronger and more unified cooperative.
Caregiver Background
At Cooperative Care, there are two primary distinctions among members: 1) between personal care and supportive home care workers; and 2) between caregivers who care for unrelated clients or family members. Many had worked as caregivers prior to joining the cooperative, either in formalized settings or in the homes of family members.
Within our sample, most client visits were of a fixed length and schedule; however, for a few clients, the schedule varied from week to week. The schedules for caregivers who took care of family members were quite different from for those who cared for unrelated clients. Caregiver who cared for family members were frequently responsible for care 24 hours a day, 7 days a week.
Caregivers reported that slightly over half (52%) of their clients were located in rural areas; the remainder (48%) were within town limits. The number of miles caregivers traveled to and from clients’ homes per week varied from one half mile to more than 300.
Equipment, Emergency Plans and Client Well-Being
Equipment. Clients used a broad array of physical devices and equipment to assist them (39 types were reported). For the majority of clients (68%), caregivers felt that they had adequate equipment. For almost a third of clients (32%), caregivers said that additional physical devices or equipment was needed, for either assisting the client or easing their own physical burden.
Suggestions for Equipment. Cooperative Care can assist clients and caregivers to obtain equipment by 1) compiling a list of possible sources of equipment; and 2) starting a “loan closet.”
Emergency Plans. Most caregivers believed that their clients’ emergency plans needed updating. Since more than half the clients lived in rural areas, some distance from the nearest hospital, caregivers said that a plan to assist their clients at their homes during an emergency was of particular importance.
Suggestions for Emergency Plans. To better address emergency situations: 1) update clients’ emergency plans for fires, storms, and medical emergencies, 2) include emergency contacts as well as other medical information; 3) depending on clients’ needs, make emergency equipment available and accessible; and 4) ensure that emergency plans are easily visible in the clients’ homes.
Client Well-Being. Due to their frequent visits, caregivers are regularly able to assess the emotional and physical state of the clients. Caregivers noted a broad range of physical, mental, and/or emotional change in clients, and had suggestions for how to improve the well-being of some clients.
Suggestions for Improving Client Well-Being. Caregivers reported that some clients are isolated and could benefit from socializing; thus, the cooperative should consider: 1) providing more opportunities for clients to socialize and have companionship; and 2) assisting clients to form support groups.
Physical and Emotional Issues Faced by Caregivers
Physical
Concerns
Physical Injuries. A minority of cooperative members had experienced physical injuries in their current clients’ homes; however, caregivers reported that there was the potential for injuries in almost half of their clients’ homes.
Suggestions for Preventing Physical Injuries. Caregivers suggested that the cooperative might: 1) obtain needed equipment for client (see Suggestions for Equipment above); 2) obtain physical devices that can be used by caregivers, such as a back brace; and 3) provide in-service training on how to use good body mechanics and equipment properly.
Pets. Pets were another potential cause for injury, as well as the cause of general anxiety for some caregivers. About half the clients had pets and about half of those clients had multiple pets.
Suggestions for Dealing with Pets. To address caregivers’ concerns about pets, the cooperative could: 1) obtain information on clients’ pets, by using new client questionnaire; and 2) draft a set of basic pet guidelines.
Emotional Concerns
Emotional Stress. Emotional stress affects caregivers who care for family members differently than those who care for unrelated clients. The major form of stress reported relates to clients’ behavior. However, family members were twice as likely to report client behavior as a problem. Cooperative members had their own, individual methods for responding to stress either on or off the job.
Suggestions for Dealing with Emotional Stress. To reduce emotional stress caregivers suggested: 1) having better communication with the cooperative office; 2) forming a support group for or assigning a mentor or support person to cooperative members; and 3) offering prizes for stress relief, perhaps at the annual meetings.
Inappropriate Behavior. Slightly over one-third of caregivers described experiences with inappropriate behavior from a client at some point during their career. Inappropriate behaviors included unwanted sexual comments or advances, hair grabbing, scratching, or general “uncomfortable situations.”
Suggestions for Dealing with Inappropriate Behavior. For caregivers to better respond to inappropriate behavior the cooperative could: 1) offer training on how to deal with this behavior; 2) ensure that staff at the cooperative office are available to discuss it; and 3) have an outside person, such as an office staff member, speak with the client instead of the caregiver to reduce the awkwardness for the caregiver.
Caregivers’ Suggestions for Building Communication and Cooperation among Cooperative Members
Cooperative members discussed four ways in which cooperative members, clients, cooperative management and the board of directors could better communicate and cooperate with each other. The suggestions included:
gathering more information about clients to give to caregivers;
establishing communication methods for caregivers who care for the same client;
creating more opportunities for cooperative members to talk with one another; and,
fostering an environment wherein cooperative members can feel more comfortable communicating with cooperative management and board of directors.
Actions
The cooperative members and staff initiated several activities after the participatory research project was completed that greatly improved membership communication and involvement, and addressed other problems identified through the research. Many factors affect changes within organizations and individuals, thus it is difficult to discern to what degree the ongoing activities and initiatives were inspired directly by the research process and its findings. However, at the very least the participatory research project “opened doors” to other activities and processes.
This report is based on a participatory research project conducted between June 2003 and December 2004, and the actions inspired by it through June 2006. The research team consisted of four members of Cooperative Care1, a worker-owned home care agency, and two academic researchers. Together these six individuals set research objectives, developed a questionnaire and consent forms, interviewed respondents, analyzed data, and disseminated research findings.
Our project was a unique case of participatory research conducted within a participatory work environment – a true exercise of democratic principles. Because other members of democratic workplaces may be inspired by participatory research methods, we describe the research process and provide links in this report to some of the tools we used in the process; we also present our major findings, and the suggestions and actions that resulted from our collaborative project.
We begin by providing some background about home care, Cooperative Care and participatory research.
Homecare Workers and Cooperative Care
The demand for home care services in the United States is growing. Most elderly people and people with disabilities who receive formal (paid) assistance receive care in their own home or other community-based settings, rather than in an institutional residential setting (12.6 million versus 1.8 million, respectively).2 As the wave of 76 million “baby boomers” (people born between 1946 and 1964 in the United States) age, the demand for paid positions in the home care sector will rise dramatically. By 2010, the number of “unskilled” home care positions is predicted to grow to 1,074,000, up from 635,000 in 2000 – an anticipated growth rate three times that of other job sectors.3
Most home care workers are self-employed or employed by non-profit or for-profit home care agencies. The quality of jobs provided by traditionally structured home care agencies is generally poor. Home care workers, the vast majority of whom are women, typically receive little or no training, earn low wages, do not have access to benefits, and work erratic hours. As a result, employee turnover in the home care industry is higher than other service sectors.
Unlike traditional home care agencies, Cooperative Care is worker-owned. The caregivers who make up its membership deliver home care services to people who are elderly and disabled in Waushara County, Wisconsin. 4 Cooperative Care’s mission statement reads:
To provide high quality home-based care to elderly people and people with disabilities while providing fair wages and benefits to the workers caring for them.
Cooperative Care – comprised of formerly independent, self-employed home care workers – opened in 2001, and, as of this writing, has approximately 85 members, all of whom are member-owners. Although a handful of cooperatively run home care agencies exist in urban areas – most prominently, in the Bronx and Philadelphia – Cooperative Care is the only one located in a rural area.
At the time this research was conducted, Cooperative Care had been in operation for less than two years, but was already receiving a great deal of local and national attention. Waushara County is a poor rural county with limited employment options. Organizing independent workers into a cooperative proved to be a good way to improve wages and benefits for home care workers and reduce worker turnover. Inspired by the national attention and success of Cooperative Care, the USDA designated $1 million in 2004 to support the further development of home care cooperatives in rural areas. Moreover, the cooperative was named as a finalist for Harvard’s John F. Kennedy Innovations in American Government Award in 2003 and 2004.
Addressing an audience of judges for the Innovations in American Government Award in 2004, Donna Tompkins, a member of Cooperative Care and president of the board at the time, (also a member of our research team) explained her cooperative this way:
We do not work for an agency; we work for ourselves as member owners of Cooperative Care. We exist as an organization for two reasons. One, we give quality care to people who need our help. Secondly, to see that our member owners are better paid - and for the first time, to have access to workers’ compensation, healthcare, holiday and overtime pay, personal time off, training, scheduling back up, and support in problem solving. We are no longer alone, having to work sick because there is no back-up, working for not much more than minimum wage, and unable to go to the doctor because there is no coverage for healthcare or work related injuries…We do not work for a corporation that will manage our funds. At Cooperative Care, all the members are the owners, and any net profit belongs to us.
Prior to the formation of the cooperative, home care workers served clients funded by the County’s Human Service Department as “independent contractors.” They earned low wages and, because they were treated as self-employed caregivers, did not receive even the most basic worker benefits, such as workers’ compensation.
Ms. Tompkin’s characterization of the cooperative as having improved their jobs and the quality of care, was a sentiment shared by other cooperative research members. They hoped that the research and its subsequent actions would enable them to improve upon their initial success. Specifically, their research objectives were to learn: 1) how the cooperative could better support its members physically and emotionally; and 2) how to improve cooperation and communication among members. The research team believed that by addressing relationship and communication concerns of workers and strengthening their organization, they could also improve the quality of the care they provided to their clients.
Worker Owned Cooperatives and Participatory Action Research
Participatory research and worker-owned cooperatives are ideally matched. Participatory research – as a method of gathering, analyzing, and distributing information – is highly democratic and empowering to individuals who, because of a lack of formal training or status as “researchers,” do not normally have the opportunity to conduct research. Participatory action research (PAR) is part of a family of common approaches that link research to social change. Although definitions vary, the one that best captures our method is the following:
A collaborative approach to inquiry or investigation that provides people with the means to take systematic action to resolve specific problems. This approach to research favors consensual and participatory procedures that enable people (a) to investigate systematically their problems and issues, (b) to formulate powerful and sophisticated accounts of their situations, and (c) to devise plans to deal with the problems at hand.5
PAR taps into local knowledge, giving voice to individuals whose ideas and concerns are critical for a full understanding of an issue. A research team whose members represent different perspectives with varied experiences within and knowledge of a community improves access to otherwise silent voices, introduces contradictory opinions, and enhances the richness of the information gathered.
Just as community involvement is a core principle of PAR, worker involvement is central to worker owned businesses. In worker-owned cooperatives, employees own and manage the business; democratic decision-making and equitable profit sharing are key components. Like PAR, worker cooperatives are participatory in that employee-members generally participate in more facets of the organization than is typical of hierarchically managed structures.
Cooperatives typically place workers in positions of power, as board and committee members, to make crucial financial and operational choices, and to share equitably in the fruits of their labor. Not only are financial rewards and risks shared among members, but also knowledge and skills related to the business and its operation are more evenly distributed among workers than is typical of other enterprises. In both PAR and worker owned enterprises, decision-making is shared with people traditionally excluded from such power in traditional (research or work) settings.
Next, we describe the research process in more detail.
Project Background
This research project consisted of five phases: training, research, analysis, feedback and action. The research team was comprised of Cooperative Care members and two academic researchers6. With the exception of the action phase (which was carried out by Cooperative Care members), each phase was carried by all the members on the research team. Each research team member’s perspective was valuable for understanding the complexities, benefits and difficulties, of caregiving in a rural county. For example, the cooperative members had years of caregiving experience with a variety of clients and organizations, but no formal research experience, while the two academic members on the team had years of research experience and no formal caregiving experience. These combined skills and perspectives contributed to and enriched the research project.
Training. In order to give all cooperative members an equal opportunity to participate in the research project, it was first announced in Cooperative Care’s monthly newsletter (see Appendix A). The notice described the project and asked for volunteers The president of the board collected names and schedules of cooperative members who inquired about the project, and set up an initial meeting with the facilitator7. Since participatory research benefits from having diverse perspectives on a research team, the academic researchers wanted to include individuals with different backgrounds and experiences. In the context of Cooperative Care, (see Chapter 2), having diverse perspectives on a team meant including members who performed either personal care or supportive care or both, members who cared for unrelated clients and those who cared for family members, and board and non-board members. Although we were able to diversify the group by position and board membership, due to the round the clock responsibilities of cooperative members who care for family members, we could not find someone who cared for family members to join the research team (see Chapter 4 for more detail).
The team had intended to start training in the Fall of 2003, however administrative issues caused them to postpone the training until Spring of 2004. After this time, the team met regularly. The training sessions (see Appendix B) consisted of team building activities, instruction on research and confidentiality, practice in a variety of data gathering techniques, and finally, development of research objectives (i.e., the major questions that the research team wanted to investigate), consent forms,8 and a questionnaire (See Appendices C9 and D). When the research team felt ready to begin interviewing, they drafted a letter to Cooperative Care members explaining the research objectives and asking for volunteers (See Appendix A).
Research. Cooperative Care has both active and inactive members; however, since the research team wanted information about caregivers’ experiences with current clients, they interviewed active members only. The research team divided the list of active members and took responsibility for making appointments to interview workers. During the interviews, the research team carefully explained the project, the objectives, and the process for maintaining confidentiality. In many instances, the research team conducted the interviews in pairs, with one interviewer asking the interview questions and a second interviewer recording the information. Cooperative team members conducted many of the interviewers; academic team members assisted occasionally. The research phase took several months to complete, during which time the research team met intermittently to discuss concerns and progress.
Analysis. Once the interviews were completed, the research team focused on analyzing the information. The analysis was accomplished in several steps. First, the research team spent a few sessions discussing each interview question and reflecting on the responses. They analyzed the information in terms of what was important and significant for the cooperative, and what responses were expected versus unexpected. These discussions were recorded on flip chart paper and the issues were prioritized. Second, the academic team members entered the interview responses into a database and printed out the responses to each question. Third, the research team carefully read the responses to each question and divided the responses into similar categories of ideas (i.e., codes).10 Finally, the research team turned the categories into visuals, such as bar graphs or pie charts, to make it easier to interpret and to explain the findings.
Feedback.11 After many months of work, the research team was excited to discuss what they had learned and to elicit feedback from cooperative members. In order to increase participation, they scheduled three feedback meetings accompanied by a meal at different times (morning, mid-day and evening) on two days. Based on the findings, the research team prepared written material to be handed out during the feedback meetings: a draft report of the initial findings, a summary, and an action plan for addressing some priority issues (see Appendix E).
At the feedback meetings, the research team presented information by topic and asked for comments regarding the findings, including suggestions and recommendations about current practices. This report incorporates these suggestions and recommendations.
Action. The conversations from the feedback meetings were the beginning of the action phase. Cooperative members gave suggestions based on the research findings and their own experiences. Cooperative members volunteered to work on some of the topics (e.g. the emergency plan and the new client questionnaire.). They hoped that these initiatives would improve the cooperative members’ satisfaction and quality of life, build a stronger cooperative, and help them better serve their clients and, finally, expand their visibility in the community to increase the number of clients served.
Organization of This Report
The remainder of this report includes the findings of the research. In particular, we present the detailed responses from the interviews of cooperative members conducted by the research team, including charts and graphs with numerical findings. In Chapters 3, 4, and 5 we include some key suggestions arising from the research and feedback meetings. In Chapter 6 we summarize the actions taken by the Cooperative following the research project and reflect on the role of the participatory research and lessons learned from the project. This report as well as appendices including invitations to participate in the project and feedback meetings, the original consent forms, questionnaire, and material shared at the feedback meetings can be accessed through web links at the University of Wisconsin-Milwaukee Center for Economic Development’s website.12
Cooperative Care Members
Distinctions Between Members
At Cooperative Care, there are two primary distinctions among members. First, there is a distinction between personal care and supportive home care workers. This distinction is based on their training and/or job responsibilities. Personal care workers are certified to provide hands-on care of clients, including bathing, feeding, and dressing (in addition to light housekeeping work). Supportive home care workers’ or “chore” workers’ job responsibilities include housekeeping tasks and yard work. The caregivers we interviewed13 reported that most of their clients received either 1) only personal care (42%); 2) some combination of personal and supportive care (38%); or 3) only supportive care (17%). A few caregivers reported providing respite (3%).
A second distinction between members is based on whether they care for unrelated clients or family members. The majority of members reported caring for unrelated clients (86%). Members who provided care for family members cared for only that client/family member, whereas other caregivers worked for multiple clients. As we illustrate in Chapter 4 of this report, the experiences of family caregivers were quite distinct from those of unrelated caregivers, especially with regard to workers’ experiences with emotional stress.
Reasons for Becoming a Caregiver
Many cooperative members had worked as caregivers prior to joining the cooperative. For example, the majority of caregivers had prior experience working as a certified nursing assistant (C.N.A) in home care, nursing home or hospital settings (see Table 2.1). Some cooperative members became caregivers prior to joining the cooperative, through previous formal or informal caregiving work, after which time they either transitioned into employment with the cooperative to continue providing care to that family member, or used the same skill set to care for an unrelated client.
Well a friend of mine said that they were looking for help and “Are you interested?” I love what I’m doing. I always did. I care for people, you know. I cared for my husband for five years. He was very sickly. And, he passed away and I just thought well “you know what you’re doing, so you might as well be doing what you’re happy about it.” I thought “ok.”
With my grandmother, I take her places. She was at the nursing homes. She had a problem here at the hospital. Then they sent her to the nursing home for 30 days and she asked me if I’d come back…[she was in a] nursing home for rehabilitation, and she asked me if I would come back and take care of her [in her home]. ..Within two weeks after that I went back.
Because my mother-in-law wanted someone to clean her house and I said I would do it for her. She actually didn’t want anybody she didn’t know to do it. So, it was nice for her that somebody that she knows to clean her house. She likes me [laughs], today.
Other cooperative members simply enjoyed working with people and thought this kind of work would be rewarding.
|
Table 2.1 How Cooperative Members Became Caregivers |
|
|
|
# of Responses |
|
Interest or expertise developed in another caregiving environment (hospital, nursing home, assisted living, home care workers through the county) |
23 |
|
Family member needed help |
9 |
|
Needed work |
9 |
|
Likes/loves helping people |
5 |
|
Influence from a friend or family member |
2 |
Working with Clients
Schedules
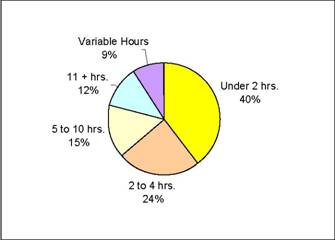
As of June 2006, cooperative members provided about 3000 hours of client care and support monthly. For the caregivers in our sample, the amount of time a caregiver spent with each client varied and depended on the caregivers’ schedules, the clients’ needs, the government reimbursement formula, and the cooperative’s scheduling process. Most of the hours the caregivers spent with the client were fixed; however, for a few clients, the schedule varied from week to week (see Figure 2.1).
Figure 2.1: Amount of Time Caregivers Spent with Each Client Per Visit

Although not distinguished in the above figure, the schedules for caregivers who took care of family members differed from those who cared for unrelated clients. Since the family member (e.g., an adult son/daughter, a husband/wife, parent or grandparent) lived with the caregiver, she or he was frequently responsible for care 24 hours a day, seven days a week (i.e., 24/7). However, it is important to note that Medicaid and Wisconsin’s in-home program for elderly and disabled people (the Community Options Program) approve the amount paid to family caregivers and often only covers a fraction of the care family members actually provide.
Travel Time
Caregivers reported that slightly over half (52%) of their clients were located in rural areas; the remainder (48%) were within town limits. The number of miles caregivers traveled to and from clients’ homes varied from one half mile to more than 300 depending on the number of clients for whom they provided care and their own residence in relation to that of their clients. As would be expected, caregivers who cared for a family member in their own home drove the least number of miles.
Cooperative Care’s clients are either elderly and/or have physical, developmental or mental disabilities. Of the 72 clients cared for by our sample of cooperative members, 55 percent were physically disabled without a developmental or mental disability and 30 percent had multiple forms of disability (e.g., physical and developmental). Over half the caregivers’ clients were women (55%) and almost half were at least 71 years of age (46%).
In order to better understand the situation of caregivers’ clients, the research team asked members about emergency plans, physical equipment and their clients’ well-being. Following each subsection, we provide caregivers’ suggestions.
Equipment
Equipment Used by Clients
Clients used a broad array of physical devices and equipment to assist them. They not only helped the client, but also assisted the caregivers (see Table 3.1).14 These devices and equipment facilitated tasks that were otherwise more physically demanding or even dangerous for the caregiver and/or client, such as moving, lifting, or bathing clients. Of the 39 types of devices used by clients, the most common were hospital beds, shower chairs, walkers and wheelchairs. A few clients had special equipment such as a voice automated computer and an electric fishing pole.
|
Table 3.1 Types of Physical Devices or Equipment Used by Clients |
|||
|
|
|||
|
Bed Rope Lift |
Elevator |
Manual Hoyer lift |
Swimming chair |
|
Cane |
Feeding pump |
Mask for sleep apnea |
Van/lift |
|
Command center |
Grab Bar/Railings |
Oxygen |
*Walker |
|
Commode |
Gait belt |
Phone holder |
*Wheelchair |
|
Donut for hips |
Handicap eating utensils |
Raised toilet seat |
|
|
Electric Hoyer lift |
Hearing aid |
Ramps |
Special Equipment |
|
Electric lift |
*Hospital bed |
Shampoo tray |
Electric fish pole |
|
Electric ramp |
Lap tray |
*Shower chair |
Electric Maid |
|
Electric scooter |
Lifeline |
Slide board |
Special shot gun |
|
Electrical wheelchair |
Lift chair Lift shoe |
Splint |
Voice automated computer |
|
|
|||
|
(* most commonly reported) |
|||
Suggestions for Clients’ Physical Devices
For the majority of clients (68%), caregivers felt that they had adequate equipment. Some reported that these needs could change over time depending on the client’s health status. For almost a third of clients (32%), caregivers said that additional physical devices or equipment were needed, either for assisting the client or easing their own physical burden. Equipment needed for clients are listed in Table 3.2.
|
Table 3.2 Additional Physical Devices or Equipment Needed by Clients |
||
|
airbed |
Hoyer lift |
raised toilet seat |
|
bigger bedroom |
lifeline |
gun holding device |
|
cane |
lift chair |
exercise device |
|
cell phone |
newer equipment |
shower chair |
|
shower in good repair |
pivot |
wheelchair |
|
four wheeler |
pull bars |
walker |
Caregivers agreed that some of their clients needed additional physical devices, and that certain clients (e.g., low income) were in more need than others, nevertheless, they were not sure that the cooperative could reasonably obtain the equipment. During the feedback meetings, cooperative members offered a number of ideas for how the cooperative could help facilitate members’ access to physical devices.
The cooperative could compile a list of possible sources of equipment. This list could be kept in the office and published in the newsletter. Equipment might be obtained through requests or purchases through churches, rummage sales, the Argus newspaper, clients’ case workers, or a neighboring county’s (e.g., Neenah’s) equipment “loan closet.”
The cooperative could start a “loan closet.” The loan closet could accept new and used equipment, including extra devises from caregivers, and lend equipment to those who need it. To facilitate the process, the cooperative might consider keeping an updated list of the types of equipment available in the loan closet.
|
Suggestions for Clients' Equipment |
|
|
Emergency Plans
Existing Emergency Plans
The research team identified the need for emergency plans as an important issue. Emergency plans must be readily available in the event of a life-threatening emergency. These situations included medical emergencies, fires, storms (e.g., tornados) and power outages. Most caregivers interviewed believed that their clients’ emergency plans needed updating. Some of the caregivers had informally developed emergency plans for their clients. For a few clients, caregivers mentioned that there was other help in the home or that the client was mobile enough to react independently to a crisis. For eleven clients, there were no emergency plans.
Power outages were of particular concern to a few caregivers whose clients were physically disabled, relied on electric equipment, and lacked alternative manual equipment. If a power outage were to occur in these homes, caregivers might find it difficult to transfer clients to safety; in some cases they would have to physically carry them out of the home or to an alternative room, such as the basement. Moreover, since more than half the clients lived in rural areas, a distance from the nearest hospital, caregivers said that a plan to assist their clients at their homes during an emergency was of particular importance.
The following emergency plans, already in place in clients’ homes, were considered helpful by the caregivers.
Phone Contacts. Caregivers liked having phone numbers easily available such as, 911, hospice, and Cooperative Care’s cell phone.
Information. Caregivers appreciated having certain information handy, such as clients’ doctor or hospital, medicine, and plans for resuscitation.
Additional Help. Another useful resource for caregivers was contact information for friends or family members who could offer assistance.
Plans. In some cases, caregivers had instructions related to a storm shelter or, if necessary, instructions for how to physically remove the client from their home if necessary – such as in the case of fire.
Caregivers reported that some clients’ homes contained emergency equipment including lifelines, phones by their beds, fire extinguishers, smoke alarms, manual Hoyer lifts, and bells in the bathrooms.
Suggestions for Improving Clients’ Emergency Plans
Caregivers had suggestions for improving emergency plans for more than half of their clients (60%).
Emergency Plans. Each client should have emergency plans for fires, storms, and medical emergencies.
Emergency contacts and medical information. Every client’s home should include readily visible information regarding emergency contacts or medical information. Information should include client’s family or friends, doctors’ phone numbers, client’s preferred hospital, list of medicines, a living will, including whether or not to resuscitate, and so forth.
Emergency equipment. Clients should have devices or
equipment to alert emergency personnel or assist with evacuation, such as
lifelines, fire extinguishers, phones, manual Hoyers, smoke alarms, or plywood.
The devices or equipment needed would depend on the physical layout of the
clients’ homes and their disabilities.
Based on these suggestions, the research team drafted an emergency plan (see Box 3.1). The plans can be individualized to fit the client’s circumstances. The information to be included in the emergency plans might be asked on the questionnaire for new clients. (For more discussion on the questionnaire for new clients, see Chapter 5.)
|
Box 3.1 Draft – Ideas for New Emergency Plans (Individualized depending on client) |
|
MEDICAL EMERGENCY |
|
1. Use lifeline (if the client has one) |
|
2. Call 911 |
|
3. Name and Location of hospital |
|
4. Dr’s name/list of meds |
|
5. Notify family contact |
|
6. Notify Cooperative |
|
STORM/TORNADO |
|
1. Identify shelter area |
|
2. Identify client transport plan |
|
3. Inventory emergency equipment (flashlight, battery, radio, oxygen?) |
|
4. Notify family contact |
|
FIRE EMERGENCY |
|
1. Check: Does the client have a smoke detector? Fire Extinguisher? |
Beyond simply collecting the information, caregivers wanted these plans to be visible and known to caregivers and nurses. Caregivers recommended keeping the information in a bright colored folder and making sure that nurses and caregivers know exactly where to find it. For example, the information could be placed in a “magnetic folder” and hung on a refrigerator.
|
Suggestions for Clients' Emergency Plans |
|
|
Client Well-Being
Assessing the Emotional and Physical State of Clients
In addition to providing physical care to clients in their homes, many cooperative members also built relationships with them. One caregiver explained,
She likes to laugh…She and I play a little game when I first get there... We do little things…That’s me. I like to get them to smile, get them to laugh, enjoy what life they have left. If they need to yell, talk, scream, whatever, [as if to her client] “Do it! That’s why I’m here, not just to give personal cares, but just someone to be there.
Due to their frequent visits, caregivers are regularly able to assess the emotional, as well as the physical, state of their clients.
According to caregivers, there is a broad range of physical, mental, and/or emotional changes in clients since they first began providing care (see Figure 3.1).
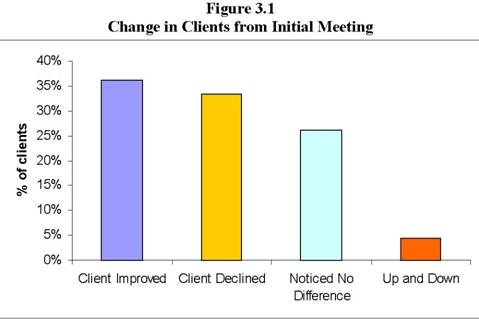
Caregivers reported that slightly over a third of clients had improved. According to caregivers, most of the improvement was in attitude and mood.
I’ve got it pretty under control. She’s getting nicer to me because she doesn’t keep all the hostility in that she had before I came…
Cooperative members said that clients who had improved were happier (11); showed signs of physical or mental improvement (9), were more talkative, (3); or had improved homes or equipment (2). However, a third of the clients had declined. Most of the decline was to physical health (14). For others, their attitudes had worsened (7); some had experienced difficult situations, such as a death of someone close or family conflict (2).
[The client has] hips hurting, depressed over the pain. Because one of the members left, she’s more lonely because this person spent a lot of time with her. It’s hard for her to turn in bed. You definitely have to help her turn in bed, because she’s hurting a lot.
Finally, about a quarter of the clients stayed relatively the same, demonstrating no difference and a few clients experienced ups and downs.
Suggestions for Improving Client Well-Being
Several caregivers had suggestions for ways to improve their clients’ or family members’ well-being (see Figure 3.2). Most commonly, caregivers felt that, because clients were often isolated, many would benefit from more socializing and companionship.
Figure 3.2
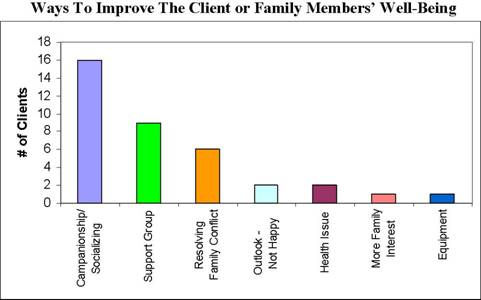
Related to companionship, caregivers recommended that clients join a support group. Support groups, members said, could be formed around clients’ talents as well as disabilities. A few caregivers felt that their clients or family members were sensitive about their disability and would feel more comfortable around others who shared it. Several caregivers also believed that family conflict was negatively affecting their clients, and that resolving it would improve their well-being. Members also mentioned that clients would benefit from improvements to their outlook, health, family interest level, or equipment access.
Caregivers at the feedback session had additional suggestions for how the county might assist isolated clients, including a recommendation that the county reinstate a “Telephone Reassurance Program” for people confined to their homes. Also, the county might allow caregivers to spend extra time with clients who need additional conversation and socializing,15 arrange for someone to visit clients in their home for some conversation in order to “get things off their chest,” or assist clients to receive home based counseling.
|
Suggestions for Improving Client Well Being |
|
|
Physical and Emotional Issues Faced by Caregivers
Most Cooperative Care members became caregivers because they enjoyed the work; nevertheless, caregiving can also involve physical and emotional demands. One of the two major objectives of this research project was to understand how the cooperative could better support its members both physically and emotionally. The research team reasoned that the first step in supporting caregivers was to obtain information about the types of physical and emotional issues Cooperative Care members face. These issues are described in this chapter.
Physical Issues for Caregivers
Job Related Injuries
Due to the physical nature of caregiving for elderly people and people with disabilities, job related injuries are common. However, only a few (4/39) Cooperative Care members had experienced physical injuries in their current clients’ homes. However, this did not mean that caregivers had not incurred injuries with previous clients or that there did not exist a potential for new injuries (see Tables 4.1 and 4.2).
Caregivers reported that there was potential for injuries in almost half of their clients’ homes, most commonly, back injuries. They believed that not using the right body mechanics or inappropriate equipment could cause injuries. Additionally, caregivers explained that sometimes, against their better judgment, they have moved something heavy for their client, such as furniture, and risked injuring themselves.
Table 4.1 Potential Injuries, by Type
Number of Responses
Back
14
Upper muscle strain
2
Scratched/draw blood
1
Table 4.2 Cause of Potential Injury
Number of Responses
Lifting (Moving Furniture, Lifting Client)
7
Not using Good Body Mechanics
3
Tripping over Animals
3
Tripping over Cords
1
Pets
Pets were another potential cause for injury, as well as the cause of general anxiety for some caregivers. About half the clients had pets and about half of those clients had multiple pets (see Figure 4.1).
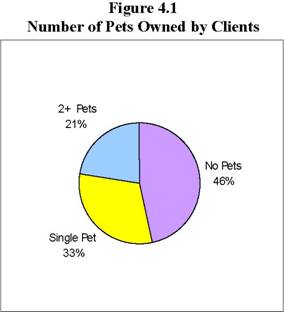
Although most members reported that pets did not affect their ability to provide care for their clients, a few expressed having problems, especially in cases of households with multiple animals. On the one hand, caregivers said that in many instances pets helped clients and were a form of comfort and companionship. On the other hand, in a minority of households, caregivers spent extra time providing care to pets, cleaning up after them, or avoiding them. They felt that this affected the time and quality of care they provided for their client. At times, it also placed the caregivers in uncomfortable situations. One caregiver explained:
You vacuum or you mop, and after you do that there’s piles of feces around on the floor… They don’t let the dogs out…. I feel that I do my work and it gets undone very fast. You know what I mean? It’s like it’s really stupid to go there. Just that I’m getting paid. There’s no additional gratification at all.
Though only a few caregivers experienced the type of unusual pet situation described above, similar problems frustrated those who regularly encountered them.
Suggestions for Dealing with Physical Concerns of Caregivers
Job Related Injuries. As suggested in Chapter 3, physical devices and equipment that assist clients can also assist caretakers and help to prevent injuries, especially injuries caused by lifting. Thus, providing all clients with the appropriate equipment can prevent the physical injuries of caregivers (see Suggestions Chapter 3). Cooperative members suggested that it would be helpful if they could notify the cooperative office if they noticed that a physical device could be useful for a client and could protect the caregiver from injury. The office could assist the caregiver by helping to locate the physical device or equipment needed by the client and caregiver.
Second, caregivers mentioned that there are physical devices that can be used by the caregiver to prevent injuries. For example, a few members reported that back braces with Velcro can prevent back injuries and can be offered to everyone who does personal and supportive care. Third, caregivers recommended having an in-service training given by an occupational or physical therapist, to refresh caregivers’ memories on how to safely use some of the equipment. The training could review how to use good body mechanics and discuss techniques on “how to say no” to certain requests (e.g., moving furniture) that may cause injury.
Pets. Suggestions on how to deal with pets prompted interest among cooperative members during the feedback session. Mainly, cooperative members found it difficult to decide on a single policy that would be right for all clients and cooperative members. Some thought that there should be clear rules concerning pets, since certain situations could cause caregivers’ stress or be detrimental to their health. Others proposed that dealing with pets should remain an individual decision, with the option for caregivers to refuse care for a pet or a client with pets.
In either case, cooperative members did agree on some useful suggestions. First, the cooperative could obtain information on clients’ pets (e.g., what type and how many) by using the new client questionnaire (see Chapter 5). Caregivers could benefit from knowing the pet situation before they begin working with a client. Second, the cooperative could draft a set of basic pet guidelines. Since each situation is different, the cooperative could use the guidelines and work with the client and caregiver to arrive at an individualized plan.
|
Suggestions for Dealing with Caregivers’ Physical Concerns |
|
To assist in preventing physical injuries the cooperative could:
obtain physical devices that could be used by caregivers. such as a back brace; and, provide in-service training on how to use good body mechanics and equipment properly. To deal with pets the cooperative could:
draft a set of basic pet guidelines. |
Emotional Issues for Caregivers
Types of Emotional Stress
Caregiving is not only physically demanding but can also be emotionally demanding as well. Due to the differences in emotional demand for family caregivers versus unrelated caregivers, these groups will be discussed separately (see Figure 4.2).16
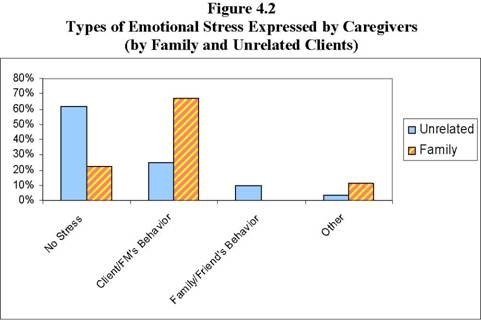
FM= Family Member
For cooperative members who cared for unrelated clients, 60 percent mentioned that they did not experience emotional stress with their clients. For those 40 percent who reported experiencing emotional stress, the more common problems were: 1) their client’s behavior (e.g., rejection of a hospital bed) or emotional state (e.g., depression); and 2) their client’s family or friend’s behavior.
The following represent some of the reactions cooperative members have had taking care of unrelated clients during stressful situations.
We’re short with the clients, and inevitability don’t provide as good a care as we should if we’re stressed out.
At the beginning he was very agitated, and having him go into a hospital bed which was just not comfortable, raising his bed, doing this, doing that, it was a little stressful, but I worked through it, I just let him use me as a sounding board and then he felt better.
[Interviewer – Was that emotionally stressful for you?]
Yeah, because you were torn between the way he felt, and the way his case worker felt, and everything else. You know someone [care worker] could get hurt, but you can understand where he’s coming from to a point. But, then he didn’t want to understand or think of us in the beginning – but now he does. Yet, he likes to play little games.
For cooperative members who cared for family members, 80 percent mentioned that they experienced emotional stress (as compared to 40 percent of caregivers who took care of unrelated clients). For both groups, client behavior was the major cause of emotional stress; however, family members were twice as likely to report it as a problem. Moreover, family caregivers reported that the level of intensity and responsibility involved in taking care of a family member was high, thus making it difficult for them to leave the family member, even for short periods.
Yes, it hurts me everyday to see him this way and feel trapped because I can't do anything and he wants me to be near… I can't leave him because he can't be alone. At times, I let him yell and get it out; he gets angry and I stay there and listen to him and try to get to the problems. He is very depressed.
We learned that the time requirement for family caregiving is caused by two mutually reinforcing tendencies. First, the family caregiver or the family member generally did not want another person caring for their family member. As said by one caregiver “he doesn't want anyone else.” Second, caregivers often felt that they knew best how to care for the family member and their needs.
An important note: The time demands of family caregiving were evident in the recruitment process for research team members. When the research project began, the research team felt it was important to include a caregiver who provided care to a family member in order to get more variety of perspectives. However, it was not possible, given the amount of time and irregular scheduling required for the project. In addition, a few caregivers expressed that it had been difficult for them to leave a family member, even for an interview or to attend the feedback meetings.
Responding to Emotional Stress
Cooperative members had their own, individual methods for responding to stress, either on or off the job. When on the job and working with a client, cooperative members usually tried to cope with the immediate situation at hand and find ways to release the stress later. During the stressful occurrences, cooperative members handled it by taking deep breaths, walking away to regain their composure, counting to 10, redirecting a conversation or a client’s behavior, or simply trying to “keep their mouth shut” and be good listeners. One cooperative member said,
… and you just have to go “ok.” Sometimes that happens. But, then I can go vent to [her husband] [laughs]. [as if to her husband] “Did you know this?” But, you just have to stay out of it. Sometimes you just have to agree or just listen. If you’re a good listener, that’s a big thing.
When off the job, cooperative members used other techniques. The most common were taking a walk, a car ride, or a trip; reading; watching television; and talking with their spouses or other caregivers. Other stress relievers included: shoveling manure, resting, calling someone, washing dishes, fishing, helping their spouse, going to church or praying, riding horses, getting beauty treatments, playing with pets, having a beer, playing on computer; writing a letter, taking medications, exercising, shopping, having lunch out, cooking, thinking through the situation that caused them the stress, changing routines, going to the park, bird watching, and feeding ducks.
Cooperative members liked the idea of getting together to discuss issues with each other, however they felt that most people are busy, making it hard to find times to meet.
Inappropriate Behavior
A few cooperative members introduced the issue of inappropriate behavior during our research team meetings, and wanted to learn more about others’ experiences. In the survey of members, we asked if they had ever experienced inappropriate behavior at any time, either during their work with the cooperative or prior to that time. It is important to note that we did not define the term “inappropriate behavior,” but instead left it open-ended for the respondents to interpret.
Although almost half of the cooperative members interviewed reported that they have never experienced inappropriate behavior, slightly over one-third described times during their career when they had experienced inappropriate behavior from a client.17 Inappropriate behavior included unwanted sexual comments or advances, hair grabbing, scratching, and just general “uncomfortable situations” (see Table 4.3).
|
Table 4.3 Inappropriate Behaviors Experienced by Caregivers
|
|
|
|
Number of Responses |
|
Inappropriate verbal interactions (i.e. yelling, sexual comments) |
10 |
|
Inappropriate physical interactions (i.e. grab hair, scratches, sexual advance) |
6 |
|
Uncomfortable situations |
3 |
Although infrequent and often excused by caregivers as caused by a client’s mental disability, such as dementia, the issue of inappropriate behavior was important for some caregivers nonetheless; caregivers needed to find methods for dealing with it. One cooperative member described her experiences and how she dealt with her client’s inappropriate behavior.
I had a couple [of experiences], and it was generally men, because of their sexual connotations, and I had to leave…and there was another elderly lady who started hallucinating and imagining that I was with her son. Then there was a personality conflict. Two men and two ladies that had personality problems.
[To resolve the problem] I tried to talk to them in a nice way, to tell them that their behavior was inappropriate, and they chose not to stop. I had to get the social workers involved and the [previous] head of here [the cooperative] to help me.
Caregivers usually dealt with this behavior themselves rather than speaking with other individuals, such as office staff, at their place of employment.
Suggestions for Dealing with Emotional Concerns of Caregivers
Reducing Emotional Stress. Most caregivers had their own, individual, methods for dealing with emotional stress, either on or off the job, and did not feel that the cooperative could play a direct role in reducing it. Nonetheless, some cooperative members did have suggestions. Most commonly mentioned were better mechanisms for communication with the office and assistance from a cooperative-sponsored support person or group. Other suggestions included having the cooperative give a gift certificate for a massage during an annual meeting, install a hot tub, or offer a relaxation class.
Responding to Inappropriate Behavior. Though many caregivers reported dealing with inappropriate behavior themselves, they had some suggestions on how the cooperative could be more involved. First, a few caregivers explained that previous training related to inappropriate behavior had helped them to know what to do or say when they had found themselves in those situations. Thus, members recommended that the cooperative include this topic in future training classes. Second, cooperative members agreed that if inappropriate behavior occurred, caregivers should feel comfortable contacting the office staff. Third, in order to prevent an uncomfortable confrontation, cooperative members said that it could be helpful to have an outside person (e.g. office staff), rather than the caregiver, speak with the client or their family.
|
Suggestions for How the Cooperative Could Assist with Caregivers’ Emotional Concerns |
|
To reduce emotional stress:
form a support group or provide a mentor or support person for cooperative members; offer prizes for stress relief. To better respond to inappropriate behavior:
ensure that cooperative members feel free to contact the office; have an outside person (e.g., office staff) speak with the client instead of the caregiver. |
Another major research objective was to find ways to build better communication and collaboration among cooperative members and thus build a more unified cooperative. Cooperative members discussed four ways in which cooperative members, clients, cooperative management and board could better communicate and cooperate with each other. They included:
gathering more information about clients to give to caregivers;
establishing communication methods for caregivers who care for the same client;
creating more opportunities for cooperative members to talk with one another; and
fostering an environment wherein cooperative members can feel more comfortable communicating with cooperative management and board of directors.
Next, we describe each of these suggestions in more detail.
Most caregivers reported that they would like to have more information about clients before they start working with them. This would serve two purposes. First, the information could enable the caregivers to provide better care to their clients. One caregiver explained the importance of initial information about clients:
[I would like to know about] health problems. I would want to know what I could do and what I can’t do, transporting them and all that, if there is any special care in… getting them out of the wheelchair, like a wheelchair lift.
A second purpose for acquiring information is to prepare workers for potentially uncomfortable home environments, in which there are protective dogs, for instance (see Chapter 4). One worker explains:
[I would want to know more about] their background, their family… and stuff like that. What kind of work they want done in their home, how they want you to do it, things they like and they don’t like. …[Also], their preferences…I guess if they have a dog that’s real protection…I’m not a real animal person. Even though I’ve been on the farm for [several years].., I don’t care about the animals, but if they’re real protective of a person, that’s scary to me for some reason…So, I don’t know if I would handle that real [well].
Specific information that caregivers reported as potentially useful are listed in Table 5.1.
|
Table 5.1 Information Caregivers Would Like to Know About New Clients |
|
|
|
# of Responses |
|
Background (marital status, age, etc.) |
11 |
|
Type of Care Expected |
11 |
|
Mental/Emotional State or Behavior |
7 |
|
Care Preferences (Routine, etc.) |
7 |
|
Disabilities/Abilities |
6 |
|
Pets |
6 |
|
Emergency Information |
5 |
|
Health Problems |
5 |
|
Medications and Side Effects |
4 |
|
Home Environment |
3 |
|
Hobbies/Interests |
3 |
|
Availability of Family |
2 |
Although the cooperative was already gathering information on new clients, the existing form would need updating in order to accommodate some of caregivers’ additional suggestions. Box 5.1 below presents a draft of ideas for a new client form compiled by research members as a result of their own experiences with new clients, as well as those of cooperative members whom they interviewed. Team members expressed that the new client form could also include questions that could be used to write the client’s emergency plans discussed in Chapter 3.
|
Box 5.1 Draft - Ideas for a New Client Form |
|
|
|
|
|
BACKGROUND |
PETS |
In addition to a client form, caregivers expressed that verbal communication is also important. For example, a few caregivers suggested it would be useful to do a “home visit” before caring for a client. They believed that an initial introduction could help put the client at ease, and better prepare the caregiver to work with the client.
|
How to and What Type of Information to Gather About Clients |
|
Establishing Communication Methods for Caregivers Who Care for the Same Client
In several instances, multiple cooperative members provided care for the same client. Members with the same client used a variety of methods for communicating with each other. The most common method was through a notebook or other note system or by speaking after a work shift or by telephone (see Table 5.2). Caregivers reported that, as clients’ health declined, more communication between caregivers was needed.
|
Table 5.2 Different Methods for Caregiver Communication |
|
|
|
# of Responses |
|
Notebook |
10 |
|
Talking after shift |
8 |
|
Telephone |
8 |
|
Leaving notes |
7 |
|
Through office staff |
1 |
|
Meeting with other workers |
1 |
|
Meetings at the office |
1 |
|
Through the client |
1 |
|
Don’t know the other members who care for the client |
1 |
Research team members recommended ways to improve communication with cooperative members who provided care for the same client. First, they suggested having social events or staff meetings for “all client team members” both for new and ongoing clients. Second, they recommended having caregivers keep notebooks with information on their client. During the discussion of these options at the feedback meeting, cooperative members mentioned several concerns related to the latter, including the importance of making decisions about how or whether to share notebooks with clients, the need to write “facts” rather then “opinions,” and the importance of using commonly accepted abbreviations. To address these concerns, some caregivers felt that the cooperative should offer a training session on keeping notebooks as a method of communication among caregivers. A few caregivers mentioned that the educational committee had already developed a client form that could be used to communicate across shifts. This could be used as a supplement to the notebooks or in place of the notebooks.
|
How to Establish Ways for Caregivers Who Care for the Same Client to Communicate |
|
Creating More Opportunities for Cooperative Members to Talk With One Another
Since caregivers work independently, they do not always have opportunities to chat or share their experiences. To remedy this, cooperative members suggested a number of possible activities. First, the cooperative could host more social activities so that cooperative members could get to know one another. Social activities could include picnics and weekly informal “lunch gatherings” at the cooperative office, where members could get to know one another. Second, the cooperative could create support groups for caregivers so they can discuss work-related issues (e.g., equipment, emotional issues, etc).
Cooperative members need to get together more often for socializing, because we hardly know each other. Not just for annual meetings [or] for bake sales. We don’t get together enough to get to know each other. Because we all have different clients, we don’t see each other, so we have different lives.
Third, cooperative members found the newsletter very valuable for keeping members informed and thought that getting information through e-mail may also be a possibility.
Cooperative members who took care of family members can feel especially isolated since it is difficult for them to find someone to substitute for them while they attend cooperative functions. This was evidenced at the feedback meeting: of the 18 cooperative members who attended only one cared for a family member. To free up time so that those family caregivers could attend social events at the cooperative, members suggested starting a volunteer respite program.
|
How to create more opportunities for cooperative members to talk with one another |
Create support group for caregivers to discuss work related issues. Consider e-mail as a method for cooperative members to communicate Start a volunteer respite program for cooperative members who take care of family members. |
Fostering an Environment Wherein Cooperative Members Feel More Comfortable Communicating With Cooperative Management and the Board Of Directors
Caregivers expressed that they want to feel comfortable communicating to the cooperative management and board regarding issues that arise with clients or the cooperative. For instance, a concern for some was the confusion surrounding “confidentiality”: what is appropriate to discuss with other caregivers or the cooperative managers. A few members said that they were concerned to talk about client issues in particular for fear of being “written up.” The confusion about the rules of confidentiality prevented some caregivers from bringing up concerns to other caregivers or to the cooperative management.
The cooperative members had three suggestions regarding confidentiality. First, the cooperative could clarify guidelines of confidentiality by using simple words. Second, the cooperative could give more frequent reminders about the rules of confidentiality, for example, as written guidelines in the newsletter. Third, the cooperative could provide a refresher class on confidentiality.
|
How to foster a more comfortable environment |
Give frequent reminders about the rules of confidentiality. Provide refresher class on confidentiality. . |
The following are some examples of the changes that occurred between January of 2005 and July 2006, based on interviews that the authors of this final report conducted with the executive director and members of the research team in July 2006, followed by some concluding reflections on the project.
Cooperative Care Activities
The cooperative members and staff initiated several activities after the participatory research project was completed that greatly improved membership communication and involvement, and addressed other problems identified through the research.
Member Communication and Involvement
Social gatherings, organized by members increased, allowing members the opportunity to get to know one another better. One member organized a pool party; others organized a picnic for cooperative members, clients and their families. A research team member said that the members welcomed these changes.
I’m happy to see that they are going on different things that people said. Like we’re having a picnic, a pool party one time, and relaxation stuff.
Another research team member noted that the involvement of members to organize some of these social activities “wouldn’t have happened three or four years ago.”
Members also formed new committees or combined existing committees to address specific organizational issues. The following are specific examples of activities initiated either by individual cooperative members or by committees:
volunteer opportunities for Habit for Humanity and a clothes drive for a local domestic violence center;
a mentor program in which after receiving training, some members acted as mentors for other members;
a process for instituting a values-based self-evaluation in which members train other members to perform self-evaluation of their work;
and, an on-call weekend coverage program.
Other issues – such as a clarification of confidentiality rules (that is, who can talk to whom about what with relation to clients) and pet guidelines – were addressed through the monthly newsletter. Significantly, and more formally, the board increased membership from five to seven members, in an effort to increase membership participation in formal decision-making.
Worker and Client Safety
A number of programs were initiated to address worker and client safety concerns that surfaced during the research. The cooperative received a grant from the Department of Health and Family Services to hire a staff member from the School of Worker’s Extension Services at the University of Wisconsin-Madison to conduct a safety survey with members and clients. The results of the survey confirmed the findings from the participatory research. Subsequently, training was conducted on worker safety and a newsletter was published with additional safety guidelines. Additionally, mentors implemented a workplace accident prevention program. Lastly, a research member solicited information about emergency planning procedures from other counties at a state conference of personal service agencies, which were being considered by the Waushara County’s Department of Human Services at the time of this writing.
Many factors affect changes within organizations and individuals. In the context of the cooperative, several changes, extraneous to the research project, occurred during and following the research that may have influenced positive changes. For instance, members gained more experience and familiarity with one another. In addition, the executive director and the board independently initiated programs, some of which were supported by grants, such as the safety evaluation and training.
It is difficult to discern, without a systematic evaluation, to what degree the ongoing activities and initiatives were inspired directly by the research process and its findings. However, research team members and the Executive Director agreed that the participatory research project “opened doors” to other activities and processes. The Executive Director remarked,
PAR exposed members to activities that they wouldn’t have been exposed to, so that when the next survey came around or when the next discussion of problems came around, they’ve already gone through this kind of process. So, I think it laid some groundwork, or at least was a precursor to the process that is in place now: open discussion, member involvement, member decision-making, that kind of thing.
The project involved a majority of cooperative members. Many cooperative members were interviewed which allowed them to assess and share their work experiences. At the feedback meetings, members reflected on the research findings which focused on other members’ experiences’ and brainstormed solutions to common problems. These experiences gave members the opportunity to voice their opinion. A research team member, also a board member, commented,
When we started to do the interviews, and get their feedback, I thought that was the first time our members had an official invitation to share their stories and their experiences. That was a really big step…[The research] opened a big door up.
The same team member felt that the research gave her an opportunity to learn about her coworkers and the situation of their clients.
I learned a lot more about health care workers, my fellow workers. I learned more about some of the situations in people’s homes, because I hadn’t had those experiences. So, sharing personal experiences with other members was a real learning process.
Another research team member said that sharing experiences facilitated communication between members and with office staff. Prior to the research, she believed that members did not feel comfortable bringing their concerns to the office staff, but instead would “just complain to one another.” Now, she said, there existed “different ways to voice [our] opinions.” We asked her if she felt the change was due to the research process. She replied,
I think it was the result of the research, because people started opening up to [the research team] and say “hey, I have a big problem,” and then people started to listen.
Lessons Learned
This project required enormous commitment of several participants’ time and energy. Administrative and scheduling complications extended the timeline of the project beyond what everyone anticipated. With the exception of one team member, who was unable to complete the project due to family caregiving responsibilities, and another who began as an observer and had not intended to take part in the interviewing and analysis, all the team members endured from start to finish.
We believe that the team stuck together and finished the project due to their personal commitments, as well as the team’s flexibility to adapt to unforeseen circumstances and work around research team members’ schedules. Ensuring an environment in which team members could fully participate, and be paid for their time and expenses, also positively contributed.18
While some events were unavoidable, it is useful to assess what might have improved the project. In short, we feel that three changes could have been made: 1) a clearer delineation of process and roles; and, 2) better communication between PAR members and other decision-makers; and, 3) ideally, a shorter time schedule.
In most participatory research projects, there are a variety of individuals representing different institutions and organizations. This was certainly the case in our project. In retrospect, we feel that the team and cooperative should have agreed to roles and responsibilities and documented for future reference.
The research process and project schedule should have been made available to office staff and to individuals in decision-making positions. This would have helped to clarify roles and responsibilities at the time of the project, and establish an institutional memory, especially important in the case of change in team members and other personnel. Periodically, there should have been opportunities to discuss the project with individuals affected by, but not directly involved in, the project, particularly those in decision-making positions.
A shorter time line would have been better for the research team members and other cooperative members to maximize momentum and ensure the usefulness of the project’s results. Our project facilitator attempted to schedule meetings on regular days and times; however, this was not always possible.19
With any project that strives to be democratic, there is an inherent tension between being inclusive and efficient. In order to have moved the project along more quickly, there would have had to have been some sacrifice to the full participation of the team members. In the end, we believe that everyone’s full participation allowed for better access to interviews and, hence, the best possible representation of the members’ experiences and opinions, resulting in a rich and interesting project.
1
See Cooperative Care’s website for more information:
www.co-opcare.com.
2
The majority of elderly people and people with disabilities in the U.S. receive
assistance exclusively through
family or friends.
3
U.S. Department of Health and Human Services, et al. 2003. The Future Supply of
Long-Term Care Workers in
Relation to the Aging Baby Boom Generation: Report to Congress. May 14.
4
The terms cooperative members, members, caregivers, and home care
workers will be used interchangeably in this report.
5 Ernest T
Stringer. 1999. Action Research, p. 17.
6
In addition, a cooperative specialist participated in our
training and occasionally attended project meetings throughout the entire
process. Though she engaged in training activities, she was not involved in the
interviewing and analysis.
7
The facilitator was one of the two academic members on the
research team.
8
Because the project was associated with the University of
Wisconsin-Milwaukee (the facilitator was employed by the university), the
research team needed approval from the university’s Institutional Review Board (IRB)
to
conduct the research. Though the IRB’s review
process helped us think more carefully about the research, it also complicated
our work and lengthened the project’s timeline by several months. Most
university IRBs do not customarily deal with PAR and are skeptical about
community members’ role in the research process. Thus, the research team faced
an evolving set of conditions to receive IRB approval. In some cases, the team
disagreed with the IRB on how the research should be conducted (e.g. the
language of the consent form), and where the research data should be stored
(e.g. the university vs. Cooperative Care). The IRB’s role in PAR is a
recurring issue for PAR practitioners working within a university setting and is
a topic of research and concern within the PAR community (See
http://www.c4qi.org/qi2006web/).
9
Originally, we had expected to interview cooperative members,
their clients and other individuals associated with the cooperative. We also
thought we would video tape some of the interviews. Each of these activities
required a separate consent form. In Appendix C, we have only included the
consent form we used for research team members and cooperative members.
10 For
example, when the cooperative members were asked ‘why they became a caregiver?’
one person might have responded that they had taken care of her mother and
another person might have taken care of her husband. These responses where
placed into a single category: “took care of a family member.”
11Another form
of feedback included presentations at one state and one international
conference, both of which were attended by cooperative and non-cooperative
members of the research team.
12
University of Wisconsin-Milwaukee Center for Economic
Development’s website: http://www.uwm.edu/Dept/CED/. The report will also be
available at Cooperative Care and can be accessed through The Center for
Cooperative’s website at the University of Wisconsin-Madison.
13
We interviewed 39 caregivers who gave responses for 72
clients. There is some minor overlap among the 39 caregivers and the clients
for whom they care; however, we were not able to account for this in our report,
because it would have required that we identify the overlap in client
assignments and break the confidentiality requirements of our study.
14Note: This
question allowed for more than one response.
15 Some
members said that in the past the county allowed extra time for caregivers to
socialize with the client, and now longer reimbursed for this.
16It should be
noted, however, that these results should be considered preliminary given the
small number (9) of family caregivers in our sample. Although a small sample,
there appear to be important differences between the emotional stresses and
needs of caregivers who provide for family members versus those who provide care
for non-family members that should be explored through further study.
17 The rest of
the cooperative members did not respond to the question.
18 The
Community Links Grant from the Wisconsin Department of Health and Family
Services covered team members’ hourly wage and mileage.
19 Caregivers’
schedules changed from week to week and the academic researchers had other
project schedules to manage.
List of Tables, Figures, and Boxes
Tables
2.1 How Cooperative Members Became Caregivers
3.1 Types of Physical Devices or Equipment Used by Clients
3.2 Additional Physical Devices or Equipment Needed by Clients
4.1 Potential Injuries, by Type
4.2 Cause of Potential Injury
4.3 Inappropriate Behaviors Experienced by Caregivers
5.1 Information Caregivers Would Like to Know About New Clients
5.2 Different Methods for Caregiver Communication
Figures
2.1 Amount of Time Caregivers Spent with Client Per Visit (in hours)
3.1 Change in Clients from Initial Meeting
3.2 Ways To Improve The Client or Family Members’ Well-Being
4.1 Number of Pets Owned by Clients
4.2 Types of Emotional Stress Expressed by Caregivers (by Family and Non-Related
Clients)
Boxes
3.1 Draft - Ideas for New Emergency Plans
5.1 Draft - Ideas for a New Client Form
Andrea Robles is a sociologist and has worked on wide array of issues using
participatory research in several African countries and in urban and rural
settings in the United States. Presently, she is working on a participatory
action research project involving community building in five economically
challenged neighborhoods in Fairfax County, Virginia with the Center for Social
Science Research at George Mason University.
Julie Whitaker earned her Ph.D. in Sociology from the University of
Wisconsin-Madison. She has assisted women form worker-owned cooperatives in the
home care sector in Wisconsin and San Miguel de Allende, Mexico, and has taught
participatory evaluation research and sociology courses.
Louise (Mankowski) Randall is a worker-owner and former board member of
Cooperative Care.
Donna Tompkins is a worker-owner and former board president of Cooperative Care
Joan Vroman is a former worker-owner of Cooperative Care.
Vicki Walejko is a worker-owner and former board member of Cooperative Care.
Margaret Bau has been a Cooperative Development Specialist with USDA Rural
Development Wisconsin since 1998.
We want to express our deep appreciation to all Cooperative Care members who have participated, taking time out of their busy lives to meet with the research team. Without you, this project would not have been possible. We hope that all the experiences you have shared will help us learn more about each other and the cooperative, and can be useful to other home care agencies and cooperatives. We also want to express our gratitude to Cooperative Care staff members, Jean Libnoch, Bonnie Starkweather, Kathie McGwin, and Pat Pintar, who assisted us and put up with our long meetings; and to Debra Takacs’ enthusiasm and her participation in the early phase of this project.
We want to give special thanks to a few people outside the cooperative who have assisted us: Lucy Rowley, now retired Director of Human Services, Waushara County who wrote the grant proposal that funded this project; Margaret Bau, a rural cooperative specialist from the USDA, who participated in the project and showed enormous interest in our work; and Lisa Heuler-Williams, at the Center for Economic Development at University of Wisconsin Milwaukee (CED-UWM), for carefully reviewing and editing the final report.
We would like to express our gratitude to the Wisconsin Department of Health and Family Services who provided financial support through a Community Links Grant that paid for our labor and materials; in particular, we sincerely thank Judy Zitske, who was so enthusiastic about our endeavor. Lastly, we want to acknowledge the Center for Economic Development at the University of Wisconsin-Milwaukee for providing additional salary funds and supporting this innovative project.